- Home
- About Us
- Membership
- Advocacy
- Whitepapers & Reports
- Ohio Council PAC
- Find My Legislators
- Ohio Medicaid Matters
- The Ohio Association for the Treatment of Opioid Dependence
- Report: 2024 School-Based Summary
- Events
- News
- Resources
- My Profile
- Key Resources for Medicaid Billing
- Key Resources for Medicaid Next Generation Implementation
- Rules Governing OhioMHAS Certified Providers
- Job Bank
|
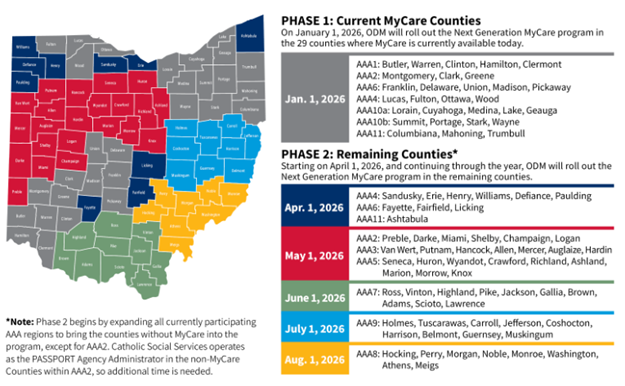
Next Generation MyCare Coming Jan 1st 2026 The Ohio Department of Medicaid (ODM) is implementing its Next Generation MyCare program beginning on January 1, 2026. MyCare Ohio is a managed care program designed for Ohioans who receive BOTH Medicaid and Medicare benefits. ODM has a Next Generation MyCare website with program updates and resources. MyCare is currently available in 29 counties and will expand statewide starting in April 2026 and concluding in August 2026.
Beginning January 1, 2026, there will be three MyCare plans available statewide.
During Medicaid or Medicare open enrollment, eligible members can pick Anthem Blue Cross and Blue Shield, CareSource, or Molina HealthCare of Ohio as their Next Generation MyCare plan.
If a member currently has a MyCare plan through Aetna or UHC, those MyCare plans will no longer be available in 2026, and they can pick a new plan during open enrollment. If a member does not pick a different plan, they will be automatically enrolled in a Next Generation MyCare plan for their Medicaid benefits. Their new plan will have as many of their current doctors as possible. A member will not lose coverage due to this change. Their Next Generation MyCare plan and benefits start on January 1, 2026. They will receive information from ODM about their new plan and options before the Next Generation MyCare program is available. If a member lives in a current MyCare Ohio County and they become eligible for MyCare before 1/1/26, they will have FFS Medicaid through the end of the calendar year. They will receive a letter between October-December 2025 that tells them their MyCare plan, when it starts, and options to change their coverage. If a member becomes eligible for MyCare after 1/1/26 and they live in a county where MyCare is not currently available, they will get a letter from ODM that provides information about their Next Generation MyCare plan, when the plan will start, and their option to change their plan. Members will receive a Next Generation MyCare ID card from their Next Generation MyCare plan as part of their member materials. If they have a MyCare Ohio plan for both their Medicaid and Medicare benefits, they have only one member ID card to be used at their appointments. If their MyCare Ohio plan only covers their Medicaid benefits, they will have up to three cards for their benefits.
In the Next Generation MyCare program, providers will be required to submit Electronic Data Interchange (EDI) transactions through the one front door, to the Ohio Medicaid Enterprise System (OMES), instead of directly to the MyCare plans. If you are submitting a claim to the plans portal using direct data entry (DDE), submit a single claim to the Next Generation MyCare plan via their existing process. If you are submitting an EDI claim for a dual benefit member (a member who gets their Medicaid and Medicare benefits from one Next Generation MyCare plan) or for a Medicaid-only member (a member who gets only Medicaid benefits from one Next Generation MyCare plan) where the Medicaid is the primary payer, submit the claim through the one front door, to the Ohio Medicaid Enterprise System (OMES). You must use the member’s Medicaid ID even if they have other ID numbers. The submitted file must use the Next Generation MyCare Plan Receiver ID and the appropriate Payer ID in the 2010BB loop for claims to be directed to the correct Next Generation MyCare plan for processing. If you are submitting an EDI claim for a Medicare covered service for a Medicaid-only member, submit the claim, also known as a crossover claim, to the primary payer.
Aetna Better Health of Ohio and United Healthcare Community Plan will no longer be MyCare plans as of December 31, 2025. They will continue to pay claims for up to 365 days from the end of the year and are responsible for any claims that have dates of service through December 31, 2025. Any claims should be submitted to Aetna or United using existing processes. Next Generation MyCare Provider Resources |